Gum Disease Treatment in Belmont WA: Early Signs and Solutions
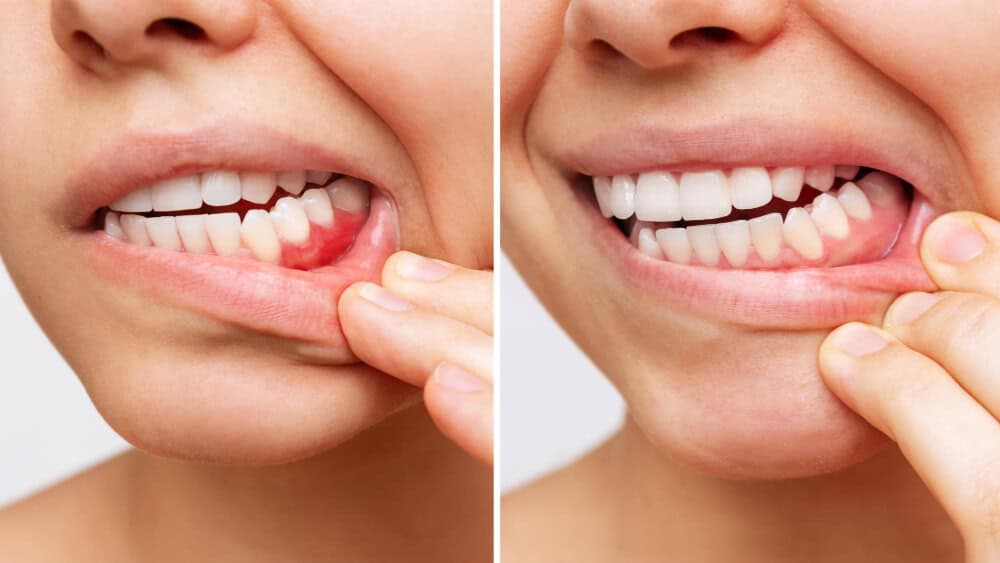
Many people don’t realise they have gum disease until it’s advanced. Red, swollen, or bleeding gums may seem minor, but they can signal a serious infection that threatens your teeth, gums, and overall health. Recognising the initial signs, knowing the underlying causes, and exploring available treatments are key to keeping your gums and teeth healthy.
While gum disease can worsen over time, timely care and consistent oral hygiene can help control symptoms and reduce the risk of tooth loss. This guide explains everything you need to know about gum disease and how treatment can help.
What Is Gum Disease?
It is a gum infection that, if ignored, can spread to the ligaments and jawbone that support your teeth. It begins subtly but can progress to a serious condition if left untreated.
How Gum Disease Develops
Plaque, or a sticky layer of bacteria, is formed on your teeth every day. Even with regular brushing, plaque can accumulate in hard-to-reach areas between teeth and along the gumline.
Plaque, over time, hardens into tartar, which cannot be removed by brushing. Bacteria in tartar release toxins that trigger inflammation, causing your gums to swell, bleed, and pull away from teeth.
Eventually, this inflammation may destroy the bone that supports your teeth and gum tissue, leading to loss of mobility and teeth unless treated.
Gingivitis vs Periodontitis
- Gingivitis: The earliest stage of gum disease. Gums can be red or swollen and even bleed during brushing or flossing. Gingivitis is reversible with proper dental care.
- Periodontitis: Advanced gum disease where gums pull away from teeth, forming pockets that collect bacteria. These pockets deepen over time, causing bone loss. Damage is often irreversible, but progression can be managed.
Prevalence
Gum disease is present in about 3 per 10 adults in Australia, and its occurrence is higher as one ages, lacks oral hygiene, smokes, or has specific medical conditions like diabetes. Preventing permanent damage involves early detection.
Early Warning Signs of Gum Disease You Shouldn’t Ignore
Recognising early symptoms allows for timely intervention before irreversible damage occurs.
- Bleeding gums: Blood when brushing or flossing is not normal and may indicate inflammation.
- Red, swollen, or tender gums: Healthy gums should be firm and pink. Persistent redness or swelling is a warning.
- Persistent bad breath (halitosis): If it continues despite brushing and flossing, it may be caused by bacterial buildup in pockets between teeth and gums.
- Receding gums: When gums pull back, teeth appear longer, and roots become exposed. This increases sensitivity to decay and the risk of decay.
- Tooth sensitivity: Exposed roots can cause sharp pain when eating hot, cold, or sweet foods.
- Loose or shifting teeth: Gum disease can damage the ligaments that hold teeth in place.
- Pain when chewing or pus between teeth and gums: Signs of infection and tissue damage.
- Changes in bite or denture fit: Teeth may move due to bone loss, affecting how your teeth meet when biting.
Tip for self-monitoring: Use a mirror to check your gums weekly. Early intervention improves treatment outcomes and preserves your smile.
Causes of Gum Disease
While bacteria in plaque are the primary cause, several factors increase susceptibility:
- Poor oral hygiene: Infrequent brushing or flossing allows plaque to accumulate.
- Smoking or tobacco use: Reduces blood flow to gums, slowing healing and increasing infection risk.
- Diabetes: A two-way relationship exists—gum disease can worsen blood sugar control, and diabetes increases susceptibility.
- Hormonal changes: Pregnancy, menopause, and menstruation can make gums more sensitive.
- Medicines: Some, such as antihistamines and antidepressants, reduce saliva, which normally protects teeth.
- Genetics: Family history can influence the risk of gum disease.
- Stress: Weakens the immune system, potentially affecting gum health.
- Poor nutrition: Deficiencies in vitamins C and D, calcium, or excessive sugar intake contribute to gum disease.
- Crooked teeth or dental appliances: Hard-to-clean areas can lead to plaque accumulation.
- Age: Risk increases after 30, and cumulative exposure to plaque over time contributes to damage.
Stages of Gum Disease: From Gingivitis to Periodontitis
- Gingivitis – Inflammation, redness, bleeding; reversible with treatment.
- Mild Periodontitis – Early bone and tissue loss, small gum pockets forming.
- Moderate Periodontitis – Deeper pockets (5–6mm), increased bone loss, potential tooth mobility.
- Severe Periodontitis – Significant bone loss, deep pockets (7mm+), loose teeth, high risk of tooth loss.
Progression timeline: Can vary from months to years depending on oral hygiene, health, and lifestyle factors.
Gum Disease Treatment Options
The treatment varies depending on the disease stage and could include:
Non-Surgical Treatments
- Professional deep cleaning (scale and clean) – Removes plaque and tartar above and below the gumline.
- Scaling and root planing – Removal of the calculus under the gum; roots are smoothed, allowing them to reattach better.
- Antimicrobial mouth rinses – Reduce bacteria in the mouth.
- Antibiotic therapy – Topical or systemic to control infection.
Surgical Treatments (for advanced cases)
- Flap surgery – Reduces pocket depth.
- Bone grafts – Rebuild lost jawbone.
- Soft tissue grafts – Cover exposed roots and improve gum health.
- Guided tissue regeneration – Stimulate growth of lost bone and tissue.
Maintenance Therapy
Ongoing care is essential:
- Periodontal cleanings every 3–4 months.
- Daily oral hygiene and self-monitoring at home.
- Modifications in lifestyle, including smoking cessation and treatment of systemic diseases.
Tip: Consistent maintenance prevents recurrence and keeps gums healthy in the long term.
How to Prevent Gum Disease
Preventive care is the most effective way to protect your gums:
- Proper brushing: Twice daily, for 2 minutes, with a soft-bristled brush at 45° to the gumline.
- Use floss or tiny brushes each day to reach the spaces between your teeth, keeping your gums healthy.
- Schedule dental visits at least every six months, and more frequently if you are prone to gum problems.
- Avoid tobacco and manage diabetes to reduce inflammation.
- Balanced diet and hydration: Nutrients support gum repair, and saliva protects teeth.
- Nightguards: Protect against teeth grinding.
- Self-checks: Look for changes in gum colour, shape, or bleeding.
The Impact of Gum Disease on Overall Well-being
Recent research shows links between gum disease and systemic conditions:
- Cardiovascular disease: Chronic inflammation may contribute to heart problems.
- Diabetes: Infection worsens blood sugar control.
- Respiratory infections: Oral bacteria can enter the lungs.
- Rheumatoid arthritis: Inflammation may be exacerbated.
- Pregnancy complications: Severe gum disease is linked to preterm birth and low birth weight.
- Alzheimer’s disease: Bacteria may influence cognitive decline.
Treating gum disease is not only about saving teeth — it may also improve overall health outcomes.
FAQ
Can gum disease be reversed?
Early-stage gingivitis can be reversed with professional cleaning and good oral hygiene. Periodontitis can be managed to prevent progression.
Is gum disease contagious?
Bacteria can spread through saliva, but developing the disease depends on your oral health and immune system.
How often should I get professional cleanings?
Every 3–4 months for those with gum disease; otherwise, every 6 months.
Can gum disease affect my heart health?
Chronic inflammation and bacteria from gum disease may enter the bloodstream, potentially influencing heart health over time. Treating gum disease can help reduce this risk.
Will I lose my teeth?
With early detection and proper treatment, most teeth can be preserved. Untreated gum disease raises the chance of tooth loss by weakening the tissue surrounding your teeth.
Does treatment hurt?
Most procedures are comfortable with anaesthetic or sedation. Minor discomfort may occur afterwards.
Can children get gum disease?
Yes, though it is less common. Helping children learn to brush and floss correctly sets the foundation for lifelong gum and tooth health.
Does bleeding gums always mean I have gum disease?
Not always, but persistent bleeding should be evaluated by your Belmont WA dentist.
Gum Disease Treatment in Belmont WA
At Epsom Dental Care, we provide personalised gum disease treatment, including early detection, professional scaling and deep cleanings, management of advanced periodontal conditions, and ongoing maintenance to help preserve your gum and tooth health.
If you are in Belmont, Rivervale, Ascot, Redcliffe, or Cloverdale, contact us on (08) 9478 2349 or visit our clinic at 5/132 Epsom Ave in Belmont WA.

